Why was oral anticoagulant (OAC) interrupted?
Was complete hemostasis achieved with no bleeding complications?
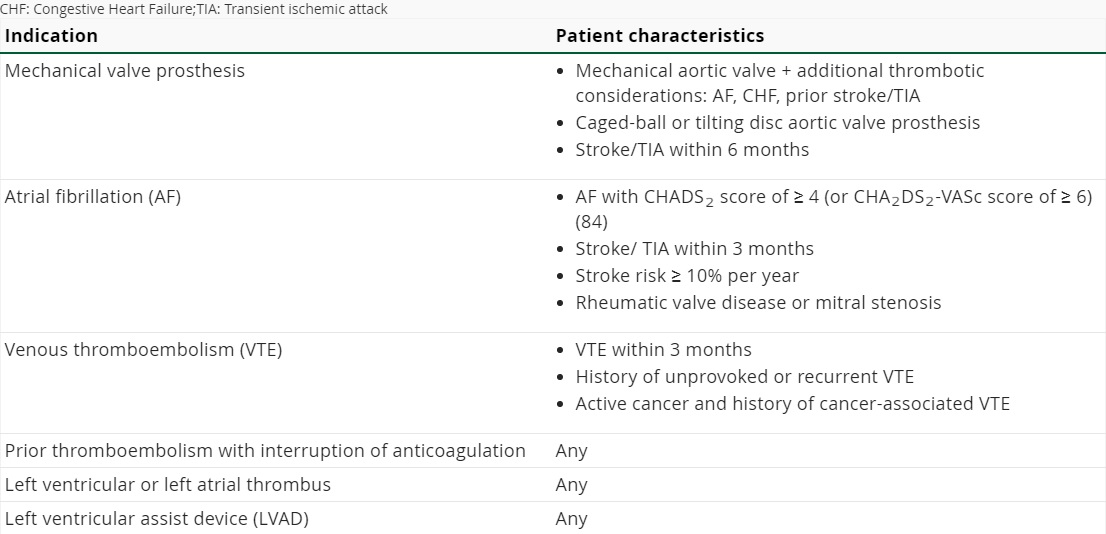
Do any of these clinical indications apply?
Based on the bleed type and clinical judgement (see info button for more), has sufficient time passed to consider restarting anticoagulation?
Based on the bleed type and clinical judgement (see info button for more), has sufficient time passed to consider restarting anticoagulation?
Is an urgent surgical/ invasive procedure planned?
Did bleeding occur at a critical site?
Is the patient at high risk of rebleeding?
Does the patient fall into 1 of the following groups?
• Nil Per Os (nothing by mouth)
• Pregnancy
• High risk of rebleeding
• Patient being bridged back to VKA with high thrombotic risk
Is the patient on concomitant antiplatelet therapy?
Is the patient taking concurrent medications that interact with OAC levels?
Does patient have nonvalvular AF?
Does > 1 of the following apply?
• High risk features of the patient
• Procedure done in a location associated with potentially catastrophic bleed
Did the patient have cardiac valve surgery?
Can patient tolerate oral medications?
What is the post-procedural bleed risk?
Is there a plan or indication to administer parenteral agent after procedure?
Does the patient fall into 1 of the following groups?
• Nil Per Os (nothing by mouth)
• High Risk of Rebleeding
• Pregnancy
What was the original anticoagulant?
Does patient have a CNS hemorrhage (e.g. ICH, spinal, ocular bleeding)?
Patients who are at high thrombotic risk will likely benefit from restarting anticoagulation, even if the risk of rebleeding is high. If there is an ongoing indication of OAC in an interrupted patient, clinicians must evaluate whether the risk of bleeding temporarily or permanently outweighs the benefit of treatment or thromboprophylaxis with OAC. The following questions help assess bleed characteristics that contribute to the risk of restarting, reversible factors that may have contributed to the bleed, indications against restarting, and indications for anticoagulation.